Hammer Toe
 Overview
Overview
A hammertoes is a toe that tends to remain bent at the middle joint in a claw-like position. There are 2 types of hammer toe. Flexible hammer toe, can be straightened by hand. Rigid hammer toe, cannot be pulled straight and can be extremely painful. The position of the toe can also lead to corns or calluses. These may also be painful. Hammer toe may be present at birth or develop later in life due to tendons that have tightened, causing the toe's joints to curl downward. Occasionally, all toes may be bent. This may be due to problems with the peripheral nerves or the spinal cord.
Causes
But what causes the imbalance of the tendons and muscles in the first place so that they begin to pull and bend the joint? A bad fitting shoe could be the cause but it usually isn?t the primary cause. Many people are genetically predisposed to hammertoe, and the condition begins to progress more quickly when they wear shoes that fit poorly, for example pointy toes, high heels, or shoes that are too short. Hammertoe may also be caused by damage to the joint as a result of trauma.
 Symptoms
Symptoms
A toe stuck in an upside-down "V" is probably a hammertoe. Some symptoms are, pain at the top of the bent toe when putting on a shoe. Corns forming on the top of the toe joint. The toe joint swelling and taking on an angry red colour. Difficulty in moving the toe joint and pain when you try to so. Pain on the ball of the foot under the bent toe. Seek medical advice if your feet regularly hurt, you should see a doctor or podiatrist. If you have a hammertoe, you probably need medical attention. Ask your doctor for a referral to a podiatrist or foot surgeon. Act now, before the problem gets worse.
Diagnosis
The exam may reveal a toe in which the near bone of the toe (proximal phalanx) is angled upward and the middle bone of the toe points in the opposite direction (plantar flexed). Toes may appear crooked or rotated. The involved joint may be painful when moved, or stiff. There may be areas of thickened skin (corns or calluses) on top of or between the toes, a callus may also be observed at the tip of the affected toe beneath the toenail. An attempt to passively correct the deformity will help elucidate the best treatment option as the examiner determines whether the toe is still flexible or not. It is advisable to assess palpable pulses, since their presence is associated with a good prognosis for healing after surgery. X-rays will demonstrate the contractures of the involved joints, as well as possible arthritic changes and bone enlargements (exostoses, spurs). X-rays of the involved foot are usually performed in a weight-bearing position.
Non Surgical Treatment
Conservative treatment is the first choice, often starting with a change of shoes to ones that have soft, larger toe spaces. Toe exercises may be prescribed to stretch and strengthen the toe muscles. Over-the-counter straps, cushions or non-medicated corn pads may be recommended to help relieve your symptoms.
Surgical Treatment
For severe hammer toe, you will need an operation to straighten the joint. The surgery often involves cutting or moving tendons and ligaments. Sometimes the bones on each side of the joint need to be connected (fused) together. Most of hammertoe the time, you will go home on the same day as the surgery. The toe may still be stiff afterward, and it may be shorter. If the condition is treated early, you can often avoid surgery. Treatment will reduce pain and walking difficulty.
 Prevention
Prevention
Wear thick-soled shoes if you walk on hard surfaces on a regular basis. Wear shoes with low heels. Have your feet checked regularly by a podiatrist to ensure that no deformities or conditions are developing. Do stretching exercises daily to strengthen the muscles in your feet.
Can Cortisone Decrease Hammer Toe Pain
hammertoe is often a harmless and hammertoe painless condition. Although the toe may be curled permanently, hammertoe should not cause any long-term problems other than a more difficult time finding shoes that fit. If hammertoe is treated and preventive measures are followed, the condition should not return. Wearing tight or constricting shoes can cause hammertoe to return.
Causes
Hammer toes can be due to a number of things. Several factors are known to increase the risk of developing hammer toes. Some people are just structurally prone to develop hammer toes (hereditary) tight footwear is an important factor in the cause of hammer toes as well as providing the pressure that causes the symptoms, weaker small muscles in the foot may also play a role.
 Symptoms
Symptoms
The symptoms of hammertoe are progressive, meaning that they get worse over time. Hammertoe causes the middle joint on the second, third, fourth, or fifth toes to bend. The affected toe may be painful or irritated, especially when you wear shoes. Areas of thickened skin (corns) may develop between, on top of, or at the end of your toes. Thickened skin (calluses) may also appear on the bottom of your toe or the ball of your foot. It may be difficult to find a pair of shoes that is comfortable to wear.
Diagnosis
The earlier a hammertoe is diagnosed, the better the prognosis and treatment options. Your doctor will be able to diagnose your hammertoe with a simple examination of the foot and your footwear. He or she may take an x-ray to check the severity of the condition. You may also be asked about your symptoms, your normal daily activities, and your medical and family history.
Non Surgical Treatment
Apply a commercial, nonmedicated hammertoe pad around the bony prominence of the hammertoe. This will decrease pressure on the area. Wear a shoe with a deep toe box. If the hammertoe becomes inflamed and painful, apply ice packs several times a day to reduce swelling. Avoid heels more than two inches tall. A loose-fitting pair of shoes can also help protect the foot while reducing pressure on the affected toe, making walking a little easier until a visit to your podiatrist can be arranged. It is important to remember that, while this treatment will make the hammertoe feel better, it does not cure the condition. A trip to the podiatric physician?s office will be necessary to repair the toe to allow for normal foot function. Avoid wearing shoes that are too tight or narrow. Children should have their shoes properly fitted on a regular basis, as their feet can often outgrow their shoes rapidly. See your podiatric physician if pain persists.
Surgical Treatment
Surgery to straighten the toe may be needed if an ulcer has formed on either the end or the top surface of the toe. Surgery sometimes involves cutting the tendons that support movement in the toe so that the toe can be straightened. Cutting the tendons, however, takes away the ability to bend the very end of the toe. Another type of surgery combines temporary insertion of a pin or rod into the toe and alteration or repair of the tendons, so that the toe is straightened. After surgery, the deformity rarely recurs.
 Prevention
Prevention
Wear thick-soled shoes if you walk on hard surfaces on a regular basis. Wear shoes with low heels. Have your feet checked regularly by a podiatrist to ensure that no deformities or conditions are developing. Do stretching exercises daily to strengthen the muscles in your feet.
What Does Over-Pronation Mean
Overview
Everyone pronates! Contrary to popular misconception it is healthy and normal. The problem begins when one or both of our feet pronate too much. When the arches flex too far inward or stay collapsed for too long pronation is considered excessive. We call this overpronation. Overpronation is by far the most common foot type. Pronation is not linked one-to-one with low arches. Although pronation lowers the arches, this does not mean that only those with low arches overpronate. People with high arches can also overpronate! Some of us have always overpronated, for others overpronation develops with age, weight gain, regular standing work or intensive exercise.

Causes
There are many biomechanical issues that can contribute to excessive pronation, including weak foot intrinsic muscles, limited ankle dorsiflexion mobility and calf flexibility, weak ankle invertor muscles (e.g. posterior tibialis), weak forefoot evertor muscles (peroneus longus), poor hip strength and control, Anterior pelvic tilting, heel InversionIn a person who overpronates, the heel bone goes into an everted position meaning that it turns out away from the midline of the body. The opposite motion of eversion is inversion. Inversion is a motion that needs to be controlled to prevent the foot from excessively pronating.
Symptoms
In addition to problems overpronation causes in the feet, it can also create issues in the calf muscles and lower legs. The calf muscles, which attach to the heel via the Achilles tendon, can become twisted and irritated as a result of the heel rolling excessively toward the midline of the body. Over time this can lead to inflexibility of the calf muscles and the Achilles tendon, which will likely lead to another common problem in the foot and ankle complex, the inability to dorsiflex. As such, overpronation is intrinsically linked to the inability to dorsiflex.
Diagnosis
To easily get an idea of whether a person overpronates, look at the position and condition of certain structures in the feet and ankles when he/she stands still. When performing weight-bearing activities like walking or running, muscles and other soft tissue structures work to control gravity's effect and ground reaction forces to the joints. If the muscles of the leg, pelvis, and feet are working correctly, then the joints in these areas such as the knees, hips, and ankles will experience less stress. However, if the muscles and other soft tissues are not working efficiently, then structural changes and clues in the feet are visible and indicate habitual overpronation.
Non Surgical Treatment
When you see the doctor, he or she will likely perform a complete examination of your feet and watch you walk. The doctor will need to take x-rays to determine the cause of your flat feet. In some cases, further imaging may be needed, especially if your symptoms are severe and sudden in nature. Once you are properly diagnosed, your doctor will create an appropriate treatment plan. There are several options to correct overpronation, such as orthotics. In many cases, overpronation can be treated with non-surgical methods and over-the-counter orthotics. In severe cases, however, custom-made orthotics may work better. Orthotics provide arch support and therefore prevent collapse of the arch with weight bearing. They are made of materials such as spongy rubber or hard plastic. Your doctor will also want to examine your footwear to ensure they fit properly and offer enough medial support. Extra support and stability can be achieved with footwear that has a firm heel counter. If you are experiencing pain, you should be able to use over-the-counter pain medications such as ibuprofen to relieve symptoms.
Prevention
Firstly, a thorough and correct warm up will help to prepare the muscles and tendons for any activity or sport. Without a proper warm up the muscles and tendons around your feet, ankles and lower legs will be tight and stiff. There will be limited blood flow to the lower legs, which will result in a lack of oxygen and nutrients for those muscles. Click here for a detailed explanation of how, why and when to perform your warm up. Secondly, flexible muscles are extremely important in the prevention of most ankle and lower leg injuries. When muscles and tendons are flexible and supple, they are able to move and perform without being over stretched. If however, your muscles and tendons are tight and stiff, it is quite easy for those muscles and tendons to be pushed beyond their natural range of motion. To keep your muscles and tendons flexible and supple, it is important to undertake a structured stretching routine.
How You Can Spot Severs Disease?
Overview
Sever?s disease is a heel problem that is the most common cause of heel pain that commonly occurs in children. It is caused by repetitive use and overuse of the heel while it is still growing, therefore is more common in active children and teenagers. Despite the name, Sever?s Disease like Osgood- Schlatter disease is caused by overuse and is not a disease.
Causes
A big tendon called the Achilles tendon joins the calf muscle at the back of the leg to the heel. Sever?s disease is thought to occur because of a mismatch in growth of the calf bones to the calf muscle and Achilles tendon. If the bones grow faster than the muscles, the Achilles tendon that attaches the muscle to the heel gets tight. At the same time, until the cartilage of the calcaneum is ossified (turned into bone), it is a potential weak spot. The tight calf muscle and Achilles tendon cause a traction injury on this weak spot, resulting in inflammation and pain. Sever?s disease most commonly affects boys aged ten to 12 years and girls aged nine to 11 years, when growth spurts are beginning. Sever?s disease heals itself with time, so it is known as self-limiting. There is no evidence to suggest that Sever?s disease causes any long term problems or complications.
Symptoms
A few signs and symptoms point to Sever?s disease, which may affect one or both heels. These include Pain at the heel or around the Achilles tendon, Heel pain during physical exercise, especially activities that require running or jumping, Worsening of pain after exercise, A tender swelling or bulge on the heel that is sore to touch, Calf muscle stiffness first thing in the morning, Limping, A tendency to tiptoe.
Diagnosis
Sever?s disease can be diagnosed based on the symptoms your child has. Your child?s doctor will conduct a physical examination by squeezing different parts of your child?s foot to see if they cause any pain. An X-ray may be used to rule out other problems, such as a broken bone or fracture.
Non Surgical Treatment
In general, management is along the normal lines for sports injuries. Simply telling an individual to give up his or her chosen sport is not satisfactory (this may be a very talented young footballer who hopes to become a professional). Explain to the child and parent that this is an overuse injury, common in the growing child. It has a good prognosis but it is necessary to ease back on training for a while to let it recover. Offer to talk to the coach. If the parent and coach are one and the same, beware that the child is being 'pushed' too hard. During abstinence from normal training, cardiovascular fitness can be maintained by non-weight-bearing exercise such as swimming or cycling.
Exercise
Exercises that help to stretch the calf muscles and hamstrings are effective at treating Sever's disease. An exercise known as foot curling, in which the foot is pointed away from the body, then curled toward the body in order to help stretch the muscles, has also proven to be very effective at treating Sever's disease. The curling exercise should be done in sets of 10 or 20 repetitions, and repeated several times throughout the day.
All You Ought To Understand About Heel Pains
Overview

Heel pain is one of the most common conditions to affect the foot. It is usually felt as an intense pain when the affected heel is used. The pain is usually worse when you get out of bed in the morning or after a long period of activity. In most cases, only one heel is affected. After walking, the pain usually improves. However, it is common for it to be painful when you first take a step after a period of rest. The pain often worsens by the end of the day. Most cases of Heel Pain are caused by damage and thickening of the plantar fascia. Sometimes, the surrounding tissue and the heel bone also become inflamed (swollen).
Causes
Heel pain is often the result of the plantar fascia being overstretched or overused. Risk factors include. Obesity or sudden weight gain. Long distance running. Tight Achilles tendons. Shoes with poor arch support or soft soles. Foot arch problems (both high arches and flat feet).
Symptoms
Pain in the bottom of the heel is the most common symptom. The pain is often described as a knife-like, pinpoint pain that is worse in the morning and generally improves throughout the day. By the end of the day the pain may be replaced by a dull ache that improves with rest. The pain results from stretching the damaged tissues. For the same reason atheletes' pain occurs during beginning stages of exercise and is relieved over time as warm-up loosens the fascia. Plantar fasciitis onset is usually gradual, only flaring up during exercise. If pain is ignored, it can eventually interfere with walking and overall, plantar fasciitis accounts for about ten percent of all running injuries.
Diagnosis
In most cases, your GP or a podiatrist (a specialist in foot problems and foot care) should be able to diagnose the cause of your heel pain by asking about your symptoms and medical history, examining your heel and foot.
Non Surgical Treatment
Treating plantar fasciitis in the early stages usually allows for a quicker recovery. Left untreated, this condition can progress to the point where there is pain with each and every step. This typically means a return to a pain free day will take much longer. Initial treatments are aimed at reducing stress on the fascia so it can begin to heal. Also, treatment to reduce the associated inflammation is started. These treatments often include: ice therapy, anti-inflammatory medications, stretching exercises, wearing shoes with appropriate support, taping of the foot and the use of a night splint. If these interventions do not lead to a full resolution, custom shoe inserts, cortisone injections and additional treatment by a physical therapist are often utilized. For patients that fail to respond to all of these efforts, surgical release of the plantar fascia can be a very effective course of action. The good news is this: 95% of the time plantar fasciitis can be fully resolved without the need for surgery. High energy shock wave therapy, sometimes referred to as orthotripsy, is a relatively new treatment that has been shown to be effective 70% of the time in patients that continue to have pain despite extensive non-surgical treatment.
Surgical Treatment
If treatment hasn't worked and you still have painful symptoms after a year, your GP may refer you to either an orthopaedic surgeon, a surgeon who specialises in surgery that involves bones, muscles and joints or a podiatric surgeon, a podiatrist who specialises in foot surgery. Surgery is sometimes recommended for professional athletes and other sportspeople whose heel pain is adversely affecting their career. Plantar release surgery is the most widely used type of surgery for heel pain. The surgeon will cut the fascia to release it from your heel bone and reduce the tension in your plantar fascia. This should reduce any inflammation and relieve your painful symptoms. Surgery can be performed either as open surgery, where the section of the plantar fascia is released by making a cut into your heel or endoscopic or minimal incision surgery - where a smaller incision is made and special instruments are inserted through the incision to gain access to the plantar fascia. Endoscopic or minimal incision surgery has a quicker recovery time, so you will be able to walk normally much sooner (almost immediately), compared with two to three weeks for open surgery. A disadvantage of endoscopic surgery is that it requires both a specially trained surgical team and specialised equipment, so you may have to wait longer for treatment than if you were to choose open surgery. Endoscopic surgery also carries a higher risk of damaging nearby nerves, which could result in symptoms such as numbness, tingling or some loss of movement in your foot. As with all surgery, plantar release carries the risk of causing complications such as infection, nerve damage and a worsening of your symptoms after surgery (although this is rare). You should discuss the advantages and disadvantages of both techniques with your surgical team.
Prevention

Make sure you wear appropriate supportive shoes. Don't over-train in sports. Make sure you warm up, cool down and undertake an exercise regime that helps maintain flexibility. Manage your weight, obesity is a factor in causing plantar fasciitis. Avoid walking and running on hard surfaces if you are prone to pain. You should follow the recognized management protocol "RICED" rest, ice, compression, elevation and diagnosis. Rest, keep off the injured ankle as much as possible. Ice, applied for 20 minutes at a time every hour as long as swelling persists. Compression, support the ankle and foot with a firmly (not tightly) wrapped elastic bandage. Elevation, keep foot above heart level to minimize bruising and swelling. Diagnosis. Consult a medical professional (such as a Podiatrist or doctor) especially if you are worried about the injury, or if the pain or swelling gets worse. If the pain or swelling has not gone down significantly within 48 hours, also seek treatment. An accurate diagnosis is essential for proper rehabilitation of moderate to severe injuries.
What Can Result In Tendinitis Discomfort In The Achilles ?
Overview
 The Achilles tendon camera.gif connects the calf muscle to the heel bone. It lets you rise up on your toes and push off when you walk or run. The two main problems are, Achilles tendinopathy. This includes one of two conditions, Tendinitis. This actually means "inflammation of the tendon." But inflammation is rarely the cause of tendon pain. Tendinosis. This refers to tiny tears (microtears) in the tissue in and around the tendon. These tears are caused by overuse. In most cases, Achilles tendon pain is the result of tendinosis, not tendinitis. Some experts now use the term tendinopathy to include both inflammation and microtears. But many doctors may still use the term tendinitis to describe a tendon injury. Problems with the Achilles tendon may seem to happen suddenly. But usually they are the result of many tiny tears in the tendon that have happened over time. Achilles tendinopathy is likely to occur in men older than 30. Most Achilles tendon ruptures occur in people 30 to 50 years old who are recreational athletes ("weekend warriors"). Ruptures can also happen in older adults.
The Achilles tendon camera.gif connects the calf muscle to the heel bone. It lets you rise up on your toes and push off when you walk or run. The two main problems are, Achilles tendinopathy. This includes one of two conditions, Tendinitis. This actually means "inflammation of the tendon." But inflammation is rarely the cause of tendon pain. Tendinosis. This refers to tiny tears (microtears) in the tissue in and around the tendon. These tears are caused by overuse. In most cases, Achilles tendon pain is the result of tendinosis, not tendinitis. Some experts now use the term tendinopathy to include both inflammation and microtears. But many doctors may still use the term tendinitis to describe a tendon injury. Problems with the Achilles tendon may seem to happen suddenly. But usually they are the result of many tiny tears in the tendon that have happened over time. Achilles tendinopathy is likely to occur in men older than 30. Most Achilles tendon ruptures occur in people 30 to 50 years old who are recreational athletes ("weekend warriors"). Ruptures can also happen in older adults.
Causes
There are several factors that can contribute to achilles tendonitis. First, you should know that the biggest contributor to chronic achilles tendonitis is ignoring pain in your achilles tendon and running through the pain of early achilles tendonitis. If your achilles tendon is getting sore it is time to pay attention to it, immediately. Sudden increases in training can contribute to achilles tendonitis. Excessive hill running or a sudden addition of hills and speed work can also contribute to this problem. Two sole construction flaws can also aggravate achilles tendonitis. The first is a sole that is too stiff, especially at the ball of the foot. (In case you are having difficulty locating the "ball" of your foot, I mean the part where the toes join the foot and at which the foot bends) If this area is stiff than the "lever arm" of the foot is longer and the achilles tendon will be under increased tension and the calf muscles must work harder to lift the heel off the ground. The second contributing shoe design factor which may lead to continuing achilles tendon problem is excessive heel cushioning. Air filled heels, while supposedly are now more resistant to deformation and leaks are not good for a sore achilles tendon. The reason for this is quite simple. If you are wearing a shoe that is designed to give great heel shock absorption what frequently happens is that after heel contact, the heel continues to sink lower while the shoe is absorbing the shock. This further stretches the achilles tendon, at a time when the leg and body are moving forward over the foot. Change your shoes to one without this "feature". Of course another major factor is excessive tightness of the posterior leg muscles, the calf muscles and the hamstrings may contribute to prolonged achilles tendonitis. Gentle calf stretching should be performed preventatively. During a bout of acute achilles tendonitis, however, overly exuberant stretching should not be performed.
Symptoms
Patients with an Achilles tendon rupture frequently present with complaints of a sudden snap in the lower calf associated with acute, severe pain. The patient reports feeling like he or she has been shot, kicked, or cut in the back of the leg, which may result in an inability to ambulate further. A patient with Achilles tendon rupture will be unable to stand on his or her toes on the affected side. Tendinosis is often pain free. Typically, the only sign of the condition may be a palpable intratendinous nodule that accompanies the tendon as the ankle is placed through its range of motion (ROM). Patients with paratenonitis typically present with warmth, swelling, and diffuse tenderness localized 2-6 cm proximal to the tendon's insertion. Paratenonitis with tendinosis. This is diagnosed in patients with activity-related pain, as well as swelling of the tendon sheath and tendon nodularity.
Diagnosis
To confirm the diagnosis and consider what might be causing the problem, it?s important to see your doctor or a physiotherapist. Methods used to make a diagnosis may include, medical history, including your exercise habits and footwear, physical examination, especially examining for thickness and tenderness of the Achilles tendon, tests that may include an x-ray of the foot, ultrasound and occasionally blood tests (to test for an inflammatory condition), and an MRI scan of the tendon.
Nonsurgical Treatment
Achilles tendonitis should never be self-treated because of the potential for permanent damage to the tendon. While you are waiting to see your doctor, however, some patients have found relief from symptoms with the use of Silipos Achilles Heel Guard during the day and a Night Splint at night. A topical pain reliever like BioFreeze Cold Therapy can provide temporary relief of pain. Achilles tendonitis only gets worse with time.

Surgical Treatment
Surgery for an acute Achilles tendon tear is seemingly straightforward. The ends of the torn tendon are surgically exposed and sutures are used to tie the ends together. The sutures used to tie together the torn tendon ends are thick and strong, and are woven into the Achilles both above and below the tear. While the concepts of surgery are straightforward, the execution is more complex. Care must be taken to ensure the tendon is repaired with the proper tension -- not too tight or too loose. The skin must be taken care of, as excessive handling of the soft tissues can cause severe problems including infection and skin necrosis. Nerves are located just adjacent to the tendon, and must be protected to prevent nerve injury. If surgery is decided upon, it is usually performed within days or weeks of the injury. The idea is to perform the repair before scar tissue has formed, which would make the repair more difficult. Some surgeons may recommend delaying surgery a few days from the initial injury to allow swelling to subside before proceeding with the repair.
Prevention
Achilles tendinitis cannot always be prevented but the following tips will help you reduce your risk. If you are new to a sport, gradually ramp up your activity level to your desired intensity and duration. If you experience pain while exercising, stop. Avoid strenuous activity that puts excessive stress on your Achilles tendon. If you have a demanding workout planned, warm up slowly and thoroughly. Always exercise in shoes that are in good condition and appropriate for your activity or sport. Be sure to stretch your calf muscles and Achilles tendon before and after working out. If you suffer from Achilles tendinitis make sure you treat it properly and promptly. If self-care techniques don?t work, don?t delay. Book a consultation with a foot care expert or you may find yourself sidelined from your favourite sports and activities.
What Is Plantar Fasciitis

Overview
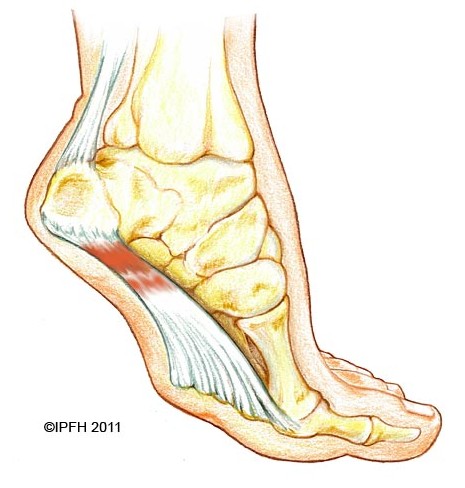
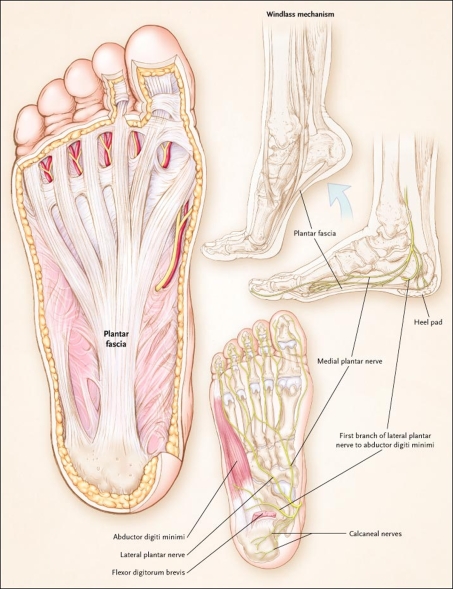
To find out where this condition gets its name, we need to look at a specific area of the foot. Your foot is made up of bones, muscles, tendons, and ligaments. The plantar fascia is a relatively inflexible, strong, fibrous band on the bottom of the foot that supports the arch of your foot. Beginning at the heel bone, the plantar fascia extends the length of your foot to connect with your toes at the ball of the foot. When you walk, your weight is distributed across your feet. Any imbalances in the mechanics of your foot and distribution of weight can potentially cause pain. Diseases involving inflammation end with "itis." This explains the name of the condition as being an inflammation of the plantar fascia, thus plantar fasciitis. Repetitive movements such as walking or running stretch the plantar fascia. Because it is not very flexible, this can cause small tears in the fascia, which leads to inflammation and pain. Other factors such as high arches, fallen arches, or a change in the walking surface contribute to the stress placed on the plantar fascia and heel.
Causes
The most frequent cause is an abnormal motion of the foot called excessive pronation. Normally, while walking or during long distance running, your foot will strike the ground on the heel, then roll forward toward your toes and inward to the arch. Your arch should only dip slightly during this motion. If it lowers too much, you have what is known as excessive pronation. For more details on pronation, please see the section on biomechanics and gait. Clinically not only those with low arches, but those with high arches can sometimes have plantar fasciitis. The mechanical structure of your feet and the manner in which the different segments of your feet are linked together and joined with your legs has a major impact on their function and on the development of mechanically caused problems. Merely having "flat feet" won't take the spring out of your step, but having badly functioning feet with poor bone alignment will adversely affect the muscles, ligaments, and tendons and can create a variety of aches and pains. Excess pronation can cause the arch of your foot to stretch excessively with each step. It can also cause too much motion in segments of the foot that should be stable as you are walking or running. This "hypermobility" may cause other bones to shift and cause other mechanically induced problems.
Symptoms
Patients with plantar fasciitis typically experience pain underneath the heel and along the inner sole of the foot. In less severe cases, patients may only experience an ache or stiffness in the plantar fascia or heel that increases with rest (typically at night or first thing in the morning) following activities which place stress on the plantar fascia. These activities typically include standing, walking or running excessively (especially up hills, on uneven surfaces or in poor footwear such as thongs), jumping, hopping and general weight bearing activity. The pain associated with this condition may also warm up with activity in the initial stages of injury. As the condition progresses, patients may experience symptoms that increase during sport or activity, affecting performance. In severe cases, patients may walk with a limp or be unable to weight bear on the affected leg. Patients with this condition may also experience swelling, tenderness on firmly touching the plantar fascia (often on a specific spot on the inner aspect of the heel) and sometimes pain on performing a plantar fascia stretch.
Diagnosis
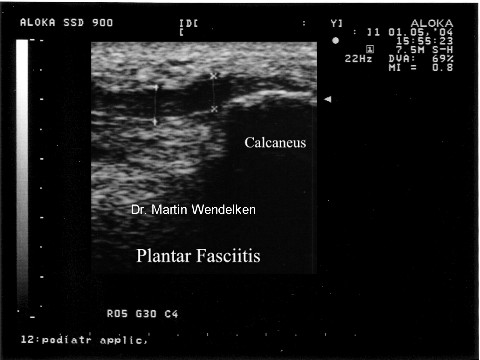
Your doctor can usually diagnose plantar fasciitis just by talking to you and examining your feet. Rarely, tests are needed if the diagnosis is uncertain or to rule out other possible causes of heel pain. These can include X-rays of the heel or an ultrasound scan of the fascia. An ultrasound scan usually shows thickening and swelling of the fascia in plantar fasciitis.
Non Surgical Treatment
Your GP or podiatrist may advise you to change your footwear. You should avoid wearing flat-soled shoes, because they will not provide your heel with support and could make your heel pain worse. Ideally, you should wear shoes that cushion your heels and provide a good level of support to the arches of your feet. For women wearing high heels, and for men wearing heeled boots or brogues, can provide short- to medium-term pain relief, as they help reduce pressure on the heels. However, these types of shoes may not be suitable in the long term, because they can lead to further episodes of heel pain. Your GP or podiatrist can advise on footwear. Orthoses are insoles that fit inside your shoe to support your foot and help your heel recover. You can buy orthoses off-the-shelf from sports shops and larger pharmacies. Alternatively, your podiatrist should be able to recommend a supplier. If your pain does not respond to treatment and keeps recurring, or if you have an abnormal foot shape or structure, custom-made orthoses are available. These are specifically made to fit the shape of your feet. However, there is currently no evidence to suggest that custom-made orthoses are more effective than those bought off-the-shelf. An alternative to using orthoses is to have your heel strapped with sports strapping (zinc oxide) tape, which helps relieve pressure on your heel. Your GP or podiatrist can teach you how to apply the tape yourself. In some cases, night splints can also be useful. Most people sleep with their toes pointing down, which means tissue inside the heel is squeezed together. Night splints, which look like boots, are designed to keep your toes and feet pointing up while you are asleep. This will stretch both your Achilles tendon and your plantar fascia, which should help speed up your recovery time. Night splints are usually only available from specialist shops and online retailers. Again, your podiatrist should be able to recommend a supplier. If treatment hasn't helped relieve your painful symptoms, your GP may recommend corticosteroid injections. Corticosteroids are a type of medication that have a powerful anti-inflammatory effect. They have to be used sparingly because overuse can cause serious side effects, such as weight gain and high blood pressure (hypertension). As a result, it is usually recommended that no more than three corticosteroid injections are given within a year in any part of the body. Before having a corticosteroid injection, a local anaesthetic may be used to numb your foot so you don't feel any pain.
Surgical Treatment
In very rare cases plantar fascia surgery is suggested, as a last resort. In this case the surgeon makes an incision into the ligament, partially cutting the plantar fascia to release it. If a heel spur is present, the surgeon will remove it. Plantar Fasciitis surgery should always be considered the last resort when all the conventional treatment methods have failed to succeed. Endoscopic plantar fasciotomy (EPF) is a form of surgery whereby two incisions are made around the heel and the ligament is being detached from the heel bone allowing the new ligament to develop in the same place. In some cases the surgeon may decide to remove the heel spur itself, if present. Just like any type of surgery, Plantar Fascia surgery comes with certain risks and side effects. For example, the arch of the foot may drop and become weak. Wearing an arch support after surgery is therefore recommended. Heel spur surgeries may also do some damage to veins and arteries of your foot that allow blood supply in the area. This will increase the time of recovery.
Prevention
The following steps will help prevent plantar fasciitis or help keep the condition from getting worse if you already have it. Take care of your feet. Wear shoes with good arch support and heel cushioning. If your work requires you to stand on hard surfaces, stand on a thick rubber mat to reduce stress on your feet. Do exercises to stretch the Achilles tendon at the back of the heel. This is especially important before sports, but it is helpful for non-athletes as well. Ask your doctor about recommendations for a stretching routine. Stay at a healthy weight for your height. Establish good exercise habits. Increase your exercise levels gradually, and wear supportive shoes. If you run, alternate running with other sports that will not cause heel pain. Put on supportive shoes as soon as you get out of bed. Going barefoot or wearing slippers puts stress on your feet. If you feel that work activities caused your heel pain, ask your human resources department for information about different ways of doing your job that will not make your heel pain worse. If you are involved in sports, you may want to consult a sports training specialist for training and conditioning programs to prevent plantar fasciitis from recurring.
What Will Cause Pain At The Heel To Appear

Overview
Foot pain affects nearly all people at one time or another. It can also lead to other musculoskeletal problems such as ankle, knee and back pain (Hill et al., 2008). This pain negatively affects one’s quality of life and ability to enjoy workouts and/or maintain a regular program of exercise. One of the most common sources of foot pain is plantar fasciitis, a condition where the connective tissue on the underside of the foot becomes irritated and painful as a result of an injury, overuse or misuse. The plantar fascia is a system of connective tissue that runs from your heel to just behind your toes. During weightbearing activities, such as walking or running, your body weight is transferred onto your foot from your heel to your toes (which results in your toes moving away from your heel). This spreading out of the foot places tension on the plantar fascia because it connects those two parts. If the tension on this structure is too great or is not dispersed evenly, the plantar fascia can develop microtears and become irritated and painful, resulting in a condition called plantar fasciitis.
Causes
Factors which may contribute to plantar fasciitis and heel spurs include a sudden increase in daily activities, increase in weight (not usually a problem with runners), or a change of shoes. Dramatic increase in training intensity or duration may cause plantar fasciitis. Shoes that are too flexible in the middle of the arch or shoes that bend before the toe joints will cause an increase in tension in the plantar fascia. Even though you may have run in shoes that are flexible before, now that you have developed plantar fasciitis, make certain that your shoe is stable and does not bend in the midfoot. Check and be certain that your shoes are not excessively worn. Shoes that do not sufficiently control excessive pronation combined with an increase in training can lead to this condition. A change in running style or parameters, such as starting speed work, running on the ball of your foot or sudden increase in hill workouts may lead to problems. All changes should be gradual and not abrupt. Gait changes such as altering your foot strike, switching shoe style, running barefoot or in minimalist shoes should all be made gradually and not abruptly. The "terrible too's" of too much, too soon, too often with too little rest also applies to "too many changes with too little adaptation". Make your changes gradually and allow your muscles, bones, and other body structures to adapt to the alterations you may be attempting.
Symptoms
Plantar fasciitis commonly causes a stabbing pain in the heel of the foot, which is worse during the first few steps of the day after awakening. As you continue to walk on the affected foot, the pain gradually lessens. Usually, only one foot is affected, but it can occur in both feet simultaneously.
Diagnosis
Plantar fasciitis is one of many conditions causing "heel pain". Some other possible causes include nerve compression either in the foot or in the back, stress fracture of the calcaneus, and loss of the fatty tissue pad under the heel. Plantar fasciitis can be distinguished from these and other conditions based on a history and examination done by a physician. It should be noted that heel spurs are often inappropriately thought to be the sole cause of heel pain. In fact, heel spurs are common and are nothing more than the bone's response to traction or pulling-type forces from the plantar fascia and other muscles in the foot where they attach to the heel bone. They are commonly present in patients without pain, and frequently absent from those who have pain. It is the rare patient who has a truly enlarged and problematic spur requiring surgery.
Non Surgical Treatment
The following self-help treatments have been found to be most effective. Rest your foot. Reduce the amount of weight-bearing activities you participate in. Get off of your feet and elevate them. This will allow healing to begin. Apply ice to your foot. Applications of ice packs that provide a comfortable cooling to the heel and arch (not a freezing cold) will help reduce pain, swelling, and inflammation. Apply the ice to the heel and arch (not the toes). Make sure it is comfortable, and leave on your foot for about 20 minutes, 3 times a day. If you have any medical problems such as diabetes, poor circulation, etc., discuss the use of ice with your doctor before applying the ice. ActiveWrap allows you to apply comfortable cold therapy to your foot without messy ice cubes. Use while on the "go." Do not walk with bare feet. Always protect your heels, arches, and plantar fascia with good supportive shoes. Orthaheel Orthotic Flip Flops For Men and Women are designed for walking comfort with built in orthotic footbeds that help reduce foot pain from plantar fasciitis. Use in the house or on the beach. Stretch the Plantar Fascia while sleeping. Plantar Fasciitis and Heel Spur pain is usually worse with the first steps in the morning. This is due to the Plantar Fascia tightening up, or contracting while we sleep. To prevent these pain producing contractures of the plantar fascia, the foot must be held in its normal or neutral position while we sleep. This optimal position of the foot is maintained with our comfortable and supportive Night Splint. When foot contractures are prevented during sleep, the "first step pains" Plantar Fasciitis and Heel Spurs will gradually subside. Stretch the Plantar Fascia during the day. Even though the Plantar Fascia is a thick tissue band with very little "give" to it, with the proper care (a Night Splint and the following exercises) it can be stretched a small amount. By stretching the Plantar Fascia even a bit, its abnormal pull on the heel is reduced. This will help to reduce pain and inflammation in the heel and arch. Two of the most effective exercises recommended are. Before stepping down, especially after sleeping or resting, stretch the arch of the foot by stretching your legs out in front of you (do not bend the knee). Place a towel around the ball of the foot. Slowly pull on the ends of the towel, pulling the toes and ball of the foot back as far as is comfortable. Hold the foot in this position for ten seconds. Repeat at least ten times. You should feel a pull on the bottom of the foot, especially in the arch. This stretches the plantar fascia, and reduces its pull on the heel. Stand about 2 to 3 feet from a wall. Lean forward with your hands against the wall. With the painful foot behind, place the other foot forward. Press against the wall, shifting weight over the front foot, while straightening the back leg. Keep the heel of the back foot on the floor and feel the stretch in the heel, Achilles tendon, and calf. Hold this position for ten seconds. Repeat at least ten times, and try to do this three times a day. When these things are achieved, the inflammation and pain of Plantar Fasciitis and Heel Spurs will gradually subside. If you are unsure of the nature of your foot problem, if your pain is intense and does not subside, if you are a diabetic or have other medical problems, if your pain is due to an injury, if an open sore is present, if a mass can be felt, or if you think that you may have an infection, we suggest that before beginning any of the above treatments you consult with your doctor.

Surgical Treatment
If treatment hasn't worked and you still have painful symptoms after a year, your GP may refer you to either an orthopaedic surgeon, a surgeon who specialises in surgery that involves bones, muscles and joints, a podiatric surgeon, a podiatrist who specialises in foot surgery. Surgery is sometimes recommended for professional athletes and other sportspeople whose heel pain is adversely affecting their career. Plantar release surgery. Plantar release surgery is the most widely used type of surgery for heel pain. The surgeon will cut the fascia to release it from your heel bone and reduce the tension in your plantar fascia. This should reduce any inflammation and relieve your painful symptoms. Surgery can be performed either as, open surgery, where the section of the plantar fascia is released by making a cut into your heel, endoscopic or minimal incision surgery - where a smaller incision is made and special instruments are inserted through the incision to gain access to the plantar fascia. Endoscopic or minimal incision surgery has a quicker recovery time, so you will be able to walk normally much sooner (almost immediately), compared with two to three weeks for open surgery. A disadvantage of endoscopic surgery is that it requires both a specially trained surgical team and specialised equipment, so you may have to wait longer for treatment than if you were to choose open surgery. Endoscopic surgery also carries a higher risk of damaging nearby nerves, which could result in symptoms such as numbness, tingling or some loss of movement in your foot. As with all surgery, plantar release carries the risk of causing complications such as infection, nerve damage and a worsening of your symptoms after surgery (although this is rare). You should discuss the advantages and disadvantages of both techniques with your surgical team. Extracorporeal shockwave therapy (EST) is a fairly new type of non-invasive treatment. Non-invasive means it does not involve making cuts into your body. EST involves using a device to deliver high-energy soundwaves into your heel. The soundwaves can sometimes cause pain, so a local anaesthetic may be used to numb your heel. It is claimed that EST works in two ways. It is thought to, have a "numbing" effect on the nerves that transmit pain signals to your brain, help stimulate and speed up the healing process. However, these claims have not yet been definitively proven. The National Institute for Health and Care Excellence (NICE) has issued guidance about the use of EST for treating plantar fasciitis. NICE states there are no concerns over the safety of EST, but there are uncertainties about how effective the procedure is for treating heel pain. Some studies have reported that EST is more effective than surgery and other non-surgical treatments, while other studies found the procedure to be no better than a placebo (sham treatment).
What Can Cause Pain At The Heel And How To End It

Overview
Heel pain is the most common musculoskeletal complaint of patients presenting to podiatric practitioners throughout the country. It is well-recognized that subcalcaneal pain syndrome, commonly attributed to plantar fascitis, is a disease entity that is increasing in its incidence, owing partly to the fact that it has a predilection for people between the age of 40 and 60, the largest age segment in our population.
Causes
When some people stand/walk/run/jump their own anatomy in their ankle joint is not ‘sturdy’ enough to cope with the needed stabilisation of their ankle joint when they are weight bearing. So, their ankle rotates to find a point of stability. By the shin twisting in and the ankle rotating downwards to the inside (along with your body weight, the power of some muscles, and of course, gravity) a huge amount of stress is applied to the plantar fascia until it is stressed beyond it’s normal limits and it starts to ‘tighten up’. It is this tightening up of the plantar fascia under this stress that causes the damage that in turn leads to pain…eventually.
Symptoms
A sharp pain in the center of your heel will most likely be one of the biggest symptoms of plantar fasciitis. A classic sign of plantar fasciitis is when the pain is worst during the first steps you take in the morning.
Diagnosis
After you describe your symptoms and discuss your concerns, your doctor will examine your foot. Your doctor will look for these signs. A high arch, an area of maximum tenderness on the bottom of your foot, just in front of your heel bone. Pain that gets worse when you flex your foot and the doctor pushes on the plantar fascia. The pain improves when you point your toes down. Limited "up" motion of your ankle. Your doctor may order imaging tests to help make sure your heel pain is caused by plantar fasciitis and not another problem. X-rays provide clear images of bones. They are useful in ruling out other causes of heel pain, such as fractures or arthritis. Heel spurs can be seen on an x-ray. Other imaging tests, such as magnetic resonance imaging (MRI) and ultrasound, are not routinely used to diagnose plantar fasciitis. They are rarely ordered. An MRI scan may be used if the heel pain is not relieved by initial treatment methods.
Non Surgical Treatment
Check your shoes to make sure they offer sufficient support and motion control. They should bend only at the ball of the foot, where your toes attach to the foot. This is very important. Avoid any shoe that bends in the center of the arch or behind the ball of the foot. It offers insufficient support and will stress your plantar fascia. The human foot was not designed to bend here and neither should a shoe be designed to do this. You may also strengthen the muscles in your arch by performing toe curls or "doming". Toe curls may be done by placing a towel on a kitchen floor and then curling your toes to pull the towel towards you. This exercise may also be done without the towel against the resistance of the floor. Plantar fasciitis is usually controlled with conservative treatment. Besides surgery and cortisone injections, physical therapy modalities such as electrical stimulation and ultrasound can be used. Often the foot will be taped to limit pronation. Following control of the pain and inflammation an orthotic (a custom made shoe insert) can be used to control over-pronation.
Surgical Treatment
Surgery is rarely used in the treatment of plantar fasciitis. However it may be recommended when conservative treatment has been tried for several months but does not bring adequate relief of symptoms. Surgery usually involves the partial release of the plantar fascia from the heel bone. In approximately 75% of cases symptoms are fully resolved within six months. In a small percentage of cases, symptoms may take up to 12 months to fully resolve.
What Is Pain In The Heel

Overview
Plantar fasciitis is a painful inflammation of the plantar fascia, a fibrous band of tissue on the bottom of the foot that helps to support the arch. Plantar fasciitis occurs when this band of tissue is overloaded or overstretched. This causes small tears in the fibers of the fascia, especially where the fascia meets the heel bone. Plantar fasciitis is common in obese people and in pregnant women, perhaps because their extra body weight overloads the delicate plantar fascia. It is also more common in people with diabetes, although the exact reason for this is unknown. Plantar fasciitis also can be triggered by physical activities that overstretch the fascia, including sports (volleyball, running, tennis), other exercises (step aerobics, stair climbing) or household exertion (pushing furniture or a large appliance). In athletes, plantar fasciitis may follow intense training, especially in runners who push themselves too quickly to run longer distances. Worn or poorly constructed shoes can contribute to the problem if they do not provide enough arch support, heel cushion or sole flexibility.
Causes
Plantar Fasciitis is frequently cited as the number one cause of heel pain. The condition affects both children and adults. Children typically outgrow the problem, but affected adults may experience recurring symptoms over the course of many months or years. The syndrome afflicts both highly active and sedentary individuals. Typically, Plantar Fasciitis results from a combination of causes, including, pronation, a condition in which the plantar fascia doesn't transfer weight evenly from the heel to the ball of the foot when you walk. Overuse of the feet without adequate periods of rest. High arches, flat feet or tightness in the Achilles' tendon at the back of the heel. Obesity. Working conditions that involve long hours spent standing or lifting heavy objects. Worn or ill-fitting footwear. The normal aging process, which can result in a loss of soft tissue elasticity. Physical trauma to the foot, as in the case of taking a fall or being involved in a car accident.
Symptoms
The symptoms of plantar fasciitis include pain in the bottom of your foot, especially at the front or centre of the heel bone, pain that is worse when first rising in the morning (called "first-step pain"), when first standing up after any long period of sitting, or after increased levels of activity especially in non-supportive shoes. Seek medical advice about plantar fasciitis if you have heel pain or pain in the bottom of your foot, especially when you get up in the morning, that does not respond to treatment or if there is redness or bruising in the heel.
Diagnosis
A physical exam performed in the office along with the diagnostic studies as an x-ray. An MRI may also be required to rule out a stress fracture, or a tear of the plantar fascia. These are conditions that do not normally respond to common plantar fasciitis treatment.
Non Surgical Treatment
Treatment initially involves offloading the plantar fascia by aoiding aggravating factors, such as running. Taping, this can work very well to alleviate pain, and can be almost immediate. It isn't a long-term solution, but can relieve symptoms in the beginning. Using a night splint to stretch the calf, so that less load is placed on the plantar fascia (if tightness in the calf is a factor). Using a gel heel cup, this can act to increase shock absorption, and by raising the heel there is also less stretch on the calf. So, temporarily, this may relieve pain in someone who has a tight calf. Massage, but this depends if the plantarfascia is actually tight or just painful. If it is tight, then massage can temporarily relieve the pain, but if it is irritated then taping and corrective footwear is preferable.
Surgical Treatment
When more-conservative measures aren't working, your doctor might recommend steroid shots. Injecting a type of steroid medication into the tender area can provide temporary pain relief. Multiple injections aren't recommended because they can weaken your plantar fascia and possibly cause it to rupture, as well as shrink the fat pad covering your heel bone. Extracorporeal shock wave therapy. In this procedure, sound waves are directed at the area of heel pain to stimulate healing. It's usually used for chronic plantar fasciitis that hasn't responded to more-conservative treatments. This procedure may cause bruises, swelling, pain, numbness or tingling and has not been shown to be consistently effective. Surgery. Few people need surgery to detach the plantar fascia from the heel bone. It's generally an option only when the pain is severe and all else fails. Side effects include a weakening of the arch in your foot.
Stretching Exercises
Stretching exercises for your foot are important. Do the stretches shown here at least twice a day. Don't bounce when you stretch. Plantar fascia stretch. To do the plantar fascia stretch, stand straight with your hands against a wall and your injured leg slightly behind your other leg. Keeping your heels flat on the floor, slowly bend both knees. You should feel the stretch in the lower part of your leg. Hold the stretch for 10 to 15 seconds. Repeat the stretch 6 to 8 times. Calf stretch. Stand with your hands against a wall and your injured leg behind your other leg. With your injured leg straight, your heel flat on the floor and your foot pointed straight ahead, lean slowly forward, bending the other leg. You should feel the stretch in the middle of your calf. Hold the stretch for 10 to 15 seconds. Repeat the stretch 6 to 8 times. Other exercises. You can also strengthen your leg muscles by standing on the ball of your foot at the edge of a step and raising up as high as possible on your toes. Relax between toe raises and let your heel fall a little lower than the edge of the step. It's also helpful to strengthen the foot by grabbing a towel with your toes as if you are going to pick up the towel with your foot. Repeat this exercise several times a day.
Workouts For Causes of Shin Splints
Did you know that redheads require 20% more general anesthesia than non-gingers before going under the knife? Often taken for granted, our feet and ankles are subjected to a rigorous workout everyday. Pain, such as may occur in our heels, alerts Heel Spur us to seek medical attention. The fungal problems seen most often are athlete's foot and fungus nails. Big toe joint pain can be a warning sign of arthritis. Enter the shape, color, or imprint of your prescription or OTC drug. Help!!!!!
Orthotics are shoe insoles, custom-made to guide the foot into corrected biomechanics. Orthotics are commonly prescribed to help with hammer toes, heel spurs, metatarsal problems, bunions, diabetic ulcerations and numerous other problems. They also help to minimize shin splints, back pain and strain on joints and ligaments. Orthotics help foot problems by ensuring proper foot mechanics and taking pressure off the parts of your foot that you are placing too much stress on. Dr. Cherine's mission is to help you realize your greatest potential and live your life to its fullest.
Most flat feet usually do not cause pain or other problems. Flat feet may be associated with pronation, a leaning inward of the ankle bones toward the center line. Foot pain, ankle pain or lower leg pain, especially in children, may be a result of flat feet and should be evaluated.

Another solution is to wear custom foot orthotics, like ezWalker ® Performance Custom Orthotics, in your shoes to help correct your body posture, stabilize your balance, relieve pain during follow-through and evenly redistribute your weight on your feet. EzWalker® Custom Orthotics are specifically made for each of your feet to properly support your arches while reducing pressure on the balls of your feet. With ezWalker® Custom Orthotics, you'll walk from lateral heel to medial forefoot for better biomechanics of your entire body. This condition manifests as a skin lesion that assumes a ring-like pattern. It can affect any region of the body, right from the scalp to the foot. One such common home remedy is the use of bleach. Many people claim that this is a very effective ringworm treatment.
Bunions are bony lumps that develop on the side of your foot and at the base of your big toe. They're the result of a condition called hallux valgus, which causes your big toe joint to bend towards your other toes and become may also develop a bursa here too, especially if your shoes press against the bunion. Sometimes swellings or bursae on the joints in your feet are also called bunions, but these aren't the same as bunions caused by hallux valgus. Hallux valgus is different to hallux rigidus, which is osteoarthritis of the big toe joint. Hallux rigidus causes your big toe to become stiff and its range of movement is reduced. Symptoms of a bunion can be controlled by choosing shoes with a soft, wide upper to reduce pressure and rubbing on your joint. Toes form hammer or claw shape.